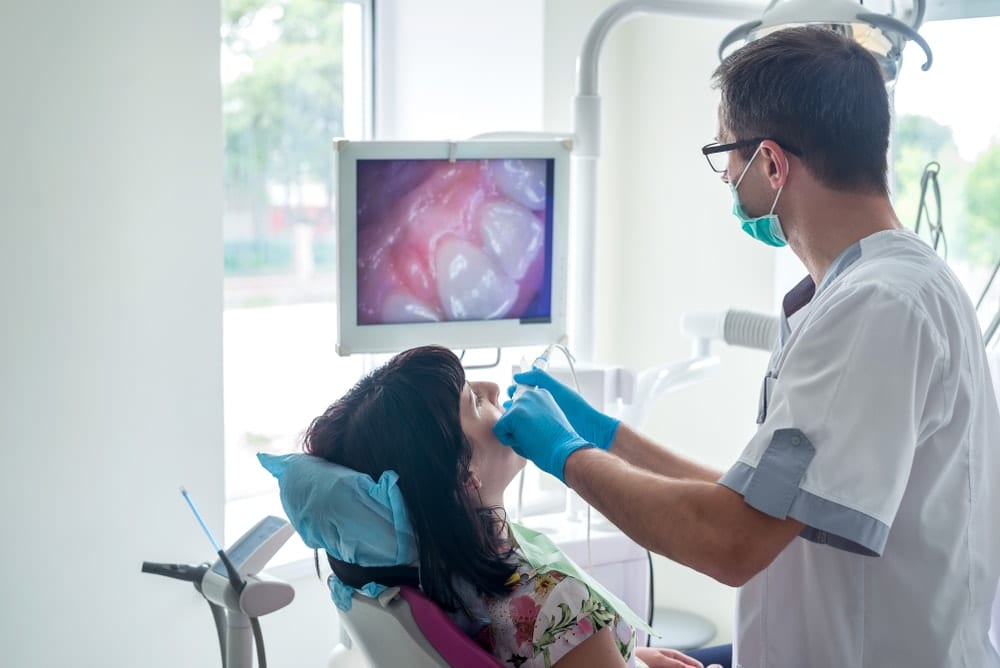
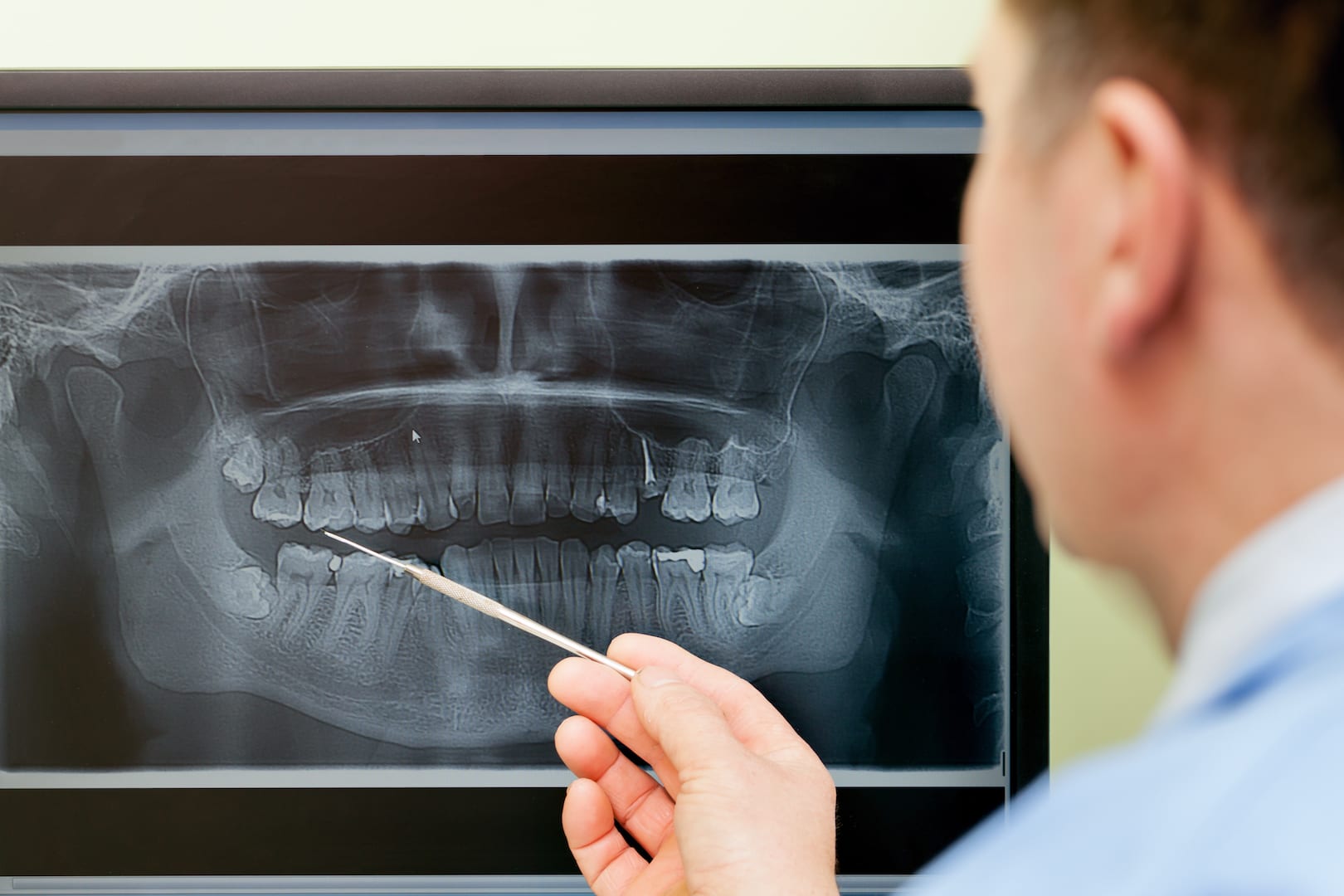
High Tech Lasers for treating Periodontal Disease
Research suggests that the use of high tech lasers as an adjunct to scaling and root planning (SRP) may improve the effectiveness of curing Periodontal Disease. In addition, when the lasers are used properly during periodontal therapy there can be less bleeding, swelling and discomfort to the patient during surgery.
A study in the Journal of Periodontology confirms findings that people with periodontal disease are at a greater risk of systemic diseases such as cardiovascular disease.
Researchers found diseased gums released significantly higher levels of bacterial pro-inflammatory components, such as endotoxins, into the bloodstream in patients with severe periodontal disease compared to healthy patients. As a result, these harmful bacterial components in the blood could travel to other organs in the body, such as the heart, and cause harm.
The study is in line with recent findings by the University of Buffalo where researchers suggest periodontal disease may cause oral bacterial components to enter the bloodstream and trigger the liver to make C-reactive proteins, which are a predictor for increased risk for cardiovascular disease.
“We found the mouth can be a major source of chronic or permanent release of toxic bacterial components in the bloodstream during normal oral functions,” said Dr. E.H. Rompen, director of the study. “This could be the missing link explaining the abnormally high blood levels of some inflammatory markers or endotoxemia observed in patients with periodontal disease.”
Researchers studied 67 patients of whom 42 were diagnosed with moderate to severe periodontitis and the remaining 25 patients were healthy individuals who had never received periodontal treatment. Blood samples were taken before and after patient’s lightly chewed chewing gum 50 times on each side of their jaw. Researchers found the number of patients with endotoxemia rose from six percent before chewing to 24 percent after chewing. Additionally, those with severe periodontal disease had approximately four times more harmful bacterial products in their blood than those with moderate or no periodontal disease.
“While this clinical study supports earlier findings, there is still much research to be done to understand the link between periodontal disease and systemic diseases, such as cardiovascular, and difficult-to-control diabetes,” “This data clearly stresses the importance of regular dental checkups to ensure a healthy, diseased-free mouth.”
Heart Disease
Several theories exist to explain the link between periodontal disease and heart disease. One theory is that oral bacteria can affect the heart when they enter the blood stream, attaching to fatty plaques in the coronary arteries (heart blood vessels) and contributing to clot formation. Coronary artery disease is characterized by a thickening of the walls of the coronary arteries due to the buildup of fatty proteins. Blood clots can obstruct normal blood flow, restricting the amount of nutrients and oxygen required for the heart to function properly. This may lead to heart attacks.
Another possibility is that the inflammation caused by periodontal disease increases plaque build up, which may contribute to swelling of the arteries.
Researchers have found that people with periodontal disease are almost twice as likely to suffer from coronary artery disease as those without periodontal disease.
Periodontal disease can also exacerbate existing heart conditions. Patients at risk for infective endocarditis may require antibiotics prior to dental procedures. Your periodontist and cardiologist will be able to determine if your heart condition requires use of antibiotics prior to dental procedures.
Stroke
Additional studies have pointed to a relationship between periodontal disease and stroke. In one study that looked at the causal relationship of oral infection as a risk factor for stroke, people diagnosed with acute cerebrovascular ischemia were found more likely to have an oral infection when compared to those in the control group.